Helicobacter Pylori
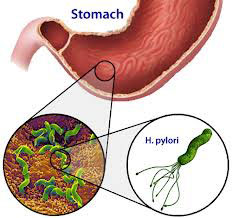
Helicobacter pylori, also known as H. pylori, is a bacterium that is commonly found in the stomach. It is present in approximately one-half of the world's population.
The vast majority of people infected with H. pylori infection have no symptoms and will never develop problems. However, H. pylori is capable of causing a number of digestive problems, including ulcers, and, much less commonly, stomach cancer. It is not clear why some people with H. pylori get these conditions and others do not.
This article discusses the symptoms, testing, and treatment of H. pylori infections. Stomach ulcers, also known as peptic ulcers, are discussed separately.
H.Pylori risk factors
H. pylori is probably spread by consuming food or water contaminated with fecal matter. H. pylori causes changes to the stomach and duodenum (the first part of the small intestine) (figure 1). The bacteria infect the protective tissue that lines the stomach. This leads to the release of certain enzymes and toxins and activation of the immune system. Together, these factors may directly or indirectly injure the cells of the stomach or duodenum. This causes chronic inflammation in the walls of the stomach (gastritis) or duodenum (duodenitis).
As a result of these changes, the stomach and duodenum are more vulnerable to damage from digestive juices, such as stomach acid.
In the United States and other developed countries, infection with H. pylori is unusual during childhood but becomes more common during adulthood. However, in developing countries, most children are infected with H. pylori before age 10.
H.Pylori symptoms
Most individuals with chronic gastritis or duodenitis have no symptoms. However, some people develop more serious problems, including stomach or duodenal ulcers.
Ulcers can cause a variety of symptoms or no symptoms at all, with the most common ulcer symptoms including:
Pain or discomfort (usually in the upper abdomen)
Bloating
Feeling full after eating a small amount of food
Lack of appetite
Nausea or vomiting
Dark or tar-colored stools
Ulcers that bleed can cause a low blood count and fatigue Less commonly, chronic gastritis causes abnormal changes in the stomach lining, which can lead to certain forms of cancer. It is uncommon to develop cancer as a result of H. pylori infection. Nevertheless, because so many people in the world are infected with H. pylori, it is considered to be an important cause of stomach cancer. People who live in countries in which H. pylori infection occurs at an early age are at greatest risk of stomach cancer.
H.Pylori diagnosis
There are several ways to diagnose H. pylori. The most commonly used tests include the following:
Blood tests — Blood tests can detect specific antibodies (proteins) that the body's immune system develops in response to the H. pylori bacterium.
Breath tests — Breath tests (known as urea breath tests) require that you drink a specialized solution containing a substance that is broken down by the H. pylori bacterium. The breakdown products can be detected in your breath.
Stool tests — Tests are available that detect H. pylori proteins in stool.
Who should be tested for H.Pylori?
If you have symptoms — Diagnostic testing for H. pylori infection isrecommended if you have active gastric or duodenal ulcers or if you have a past history of ulcers.
Although H. pylori infection is the most common cause of ulcers, not all patients with ulcers have H. pylori. Certain medications (eg, aspirin, ibuprofen [Motrin, Advil], naproxen [Aleve]) can also cause peptic ulcers.
If you do not have symptoms — H. pylori testing is usually not recommended if you have no symptoms and no past history of peptic ulcer disease. However, it may be considered for selected people, such as those with a family history or concern about stomach cancer, particularly individuals of Chinese, Korean, Japanese, or Central American descent; these groups have a higher incidence of stomach cancer.
H.Pylori treatment
People with a history of peptic ulcer disease, active gastric ulcer, or active duodenal ulcer associated with H. pylori infection should be treated. Successful treatment of H. pylori can help the ulcer to heal, prevent ulcers from coming back, and reduce the risk of ulcer complications (like bleeding).
Medications — No single drug cures H. pylori infection. Treatment involves taking several medications for 7 to 14 days.
Most of the treatment regimens include a medication called a proton pump inhibitor. This medication decreases the stomach's production of acid, which allows the tissues damaged by the infection to heal. Examples of proton pump inhibitors include lansoprazole (Prevacid), omeprazole (Prilosec), pantoprazole (Protonix), rabeprazole (AcipHex), dexlansoprazole (Dexilant), and esomeprazole (Nexium).
Two antibiotics are also generally recommended; this reduces the risk of treatment failure and antibiotic resistance.
There are increasing numbers of patients with H. pylori infection that is resistant to antibiotics so it is important to take all the medications prescribed and to have a test that confirms that the infection has been cleared.
Although the optimal H. pylori treatment regimen continues to be investigated, the American College of Gastroenterology has recommended four specific drug regimens that use a combination of at least three medications. These regimens successfully cure infection in up to 90 percent of people. For the H. pylori treatment to be effective, it is important to take the entire course of all medications.
Side effects — Up to 50 percent of patients have side effects while taking H. pylori treatment. Side effects are usually mild, and fewer than 10 percent of patients stop treatment because of side effects. For those who do experience side effects, it may be possible to make adjustments in the dose or timing of medication. Some of the most common side effects are described below.
Some of the treatment regimens use a medication called metronidazole (Flagyl) or clarithromycin (Biaxin). These medications can cause a metallic taste in the mouth.
Alcoholic beverages (eg, beer, wine) should be avoided while taking metronidazole; the combination can cause skin flushing, headache, nausea, vomiting, sweating and a rapid heart rate.
Bismuth, which is contained in some of the regimens, causes the stool to become black and may cause constipation.
Many of the regimens cause diarrhea and stomach cramps.
Treatment failure — Up to 20 percent of patients with H. pylori infection are not cured after completing their first course of treatment. A second treatment regimen is usually recommended in this case. Retreatment usually requires that the patient take 14 days of a proton pump inhibitor and two antibiotics. At least one of the antibiotics is different from those used in the first treatment course.
Follow-up — After completing H. pylori treatment, repeat testing is usually performed to ensure that the infection has resolved. This is typically done with a breath or stool test (see 'Breath tests' above). Blood tests are not recommended for follow up testing; the antibody detected by the blood test often remains in the blood for four or more months after treatment, even after the infection is eliminated.
Summary
Helicobacter pylori, also known as H. pylori, is a bacterium that is commonly found in the stomach. Most people infected with H. pylori infection have no problems. However, some people develop problems, such as stomach ulcers.
Ulcers may cause no symptoms, or may cause pain or discomfort (usually in the upper abdomen), bloating, feeling full after eating a small amount of food, lack of appetite, nausea, vomiting, and dark or tar-colored stools. Ulcers that bleed can cause a low blood count.
H. pylori can be diagnosed with a test of the blood, breath, or stool.
H. pylori testing is recommended for anyone with a peptic (stomach or duodenal) ulcer.
Anyone diagnosed with H. pylori should be treated. H. pylori treatment helps to heal the ulcer, lowers the risk that the ulcer will return, and lowers the risk of bleeding from the ulcer.
H. pylori treatment usually includes several medicines. At least two of the medicines are antibiotics that help to kill the bacteria. The other medication causes the stomach to make less acid; lower acid levels help the ulcer to heal.
Most people are cured after finishing one to two weeks of medicine. Some people need to take another two weeks of medicine. It is important to finish all of the medicine to ensure that the bacteria are killed.
A breath or stool test is usually done after finishing the medication. This is done to be sure that the bacteria were killed.