Pancreatic Cancer
What is Pancreatic Cancer?
Pancreatic cancer is a tumor of the pancreas. The pancreas is a gland located deep in the abdomen (belly) between the stomach and the spine (backbone). The liver, intestine, and other organs surround the pancreas. The pancreas is about 6 inches long and is shaped like a banana. The widest part of the pancreas is the head, the middle section is the body, and the thinnest part is the tail.
The pancreas makes insulin and other hormones. These hormones enter the bloodstream and travel throughout the body. They help the body use or store the energy that comes from food. For example, insulin helps control the amount of sugar in the blood.
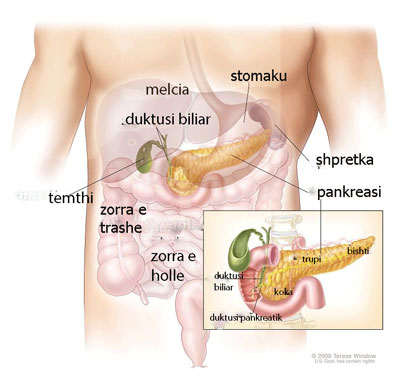 The pancreas also makes pancreatic juices. These juices contain enzymes that help digest food. The pancreas releases the juices into a system of ducts leading to the common bile duct. The common bile duct empties into the duodenum, the first section of the small intestine.
The pancreas also makes pancreatic juices. These juices contain enzymes that help digest food. The pancreas releases the juices into a system of ducts leading to the common bile duct. The common bile duct empties into the duodenum, the first section of the small intestine.
Cancer is a group of many related diseases. All cancers begin in cells, the body's basic unit of life. Cells make up tissues, and tissues make up the organs of the body. Normally, cells grow and divide to form new cells as the body needs them. When cells grow old and die, new cells take their place. Sometimes this orderly process breaks down. New cells form when the body does not need them, or old cells do not die when they should. These extra cells can form a mass of tissue called a growth or tumor.
Tumors can be benign or malignant:
Benign tumors are not cancerous. Usually, doctors can remove them. In most cases, benign tumors do not come back after they are removed. Cells from benign tumors do not spread to tissues around them or to other parts of the body. Most importantly, benign tumors are rarely a threat to life.
Malignant tumors are cancerous. They are generally more serious and may be life threatening. Cancer cells can invade and damage nearby tissues and organs. Also, cancer cells can break away from a malignant tumor and enter the bloodstream or lymphatic system. That is how cancer cells spread from the original cancer (primary tumor) to form new tumors in other organs. The spread of cancer is called metastasis.
Most pancreatic cancers begin in the ducts that carry pancreatic juices. Cancer of the pancreas may be called pancreatic cancer or carcinoma of the pancreas.
When cancer of the pancreas spreads ( metastasizes) outside the pancreas, cancer cells are often found in nearby lymph nodes. If the cancer has reached these nodes, it means that cancer cells may have spread to other lymph nodes or other tissues, such as the liver or lungs. Sometimes cancer of the pancreas spreads to the peritoneum, the tissue that lines the abdomen.
When cancer spreads from its original place to another part of the body, the new tumor has the same kind of abnormal cells and the same name as the primary tumor. For example, if cancer of the pancreas spreads to the liver, the cancer cells in the liver are pancreatic cancer cells. The disease is metastatic pancreatic cancer, not liver cancer. It is treated as pancreatic cancer, not liver cancer.
Pancreatic Cancer: Who's at risk?
The exact cause is unknown. It is slightly more common in men than in women. The risk increases with age.
It is more common in smokers and in obese (very overweight) individuals.
Almost 1/3 of cases of pancreatic carcinoma can be traced to cigarette smoking. However, it is clear that this disease is not contagious. No one can "catch" cancer from another person.
Research has shown that people with certain risk factors are more likely than others to develop pancreatic cancer. A risk factor is anything that increases a person's chance of developing a disease.
Some risk factors are:
 Age - The likelihood of developing pancreatic cancer increases with age. Most pancreatic cancers occur in people over the age of 60.
Age - The likelihood of developing pancreatic cancer increases with age. Most pancreatic cancers occur in people over the age of 60.
Smoking - Cigarette smokers are two or three times more likely than nonsmokers to develop pancreatic cancer.
Diabetes - Pancreatic cancer occurs more often in people who have diabetes than in people who do not.
Being male - More men than women are diagnosed with pancreatic cancer.
Being African American - African Americans are more likely than Asians, Hispanics, or whites to get pancreatic cancer.
Family history - The risk for developing pancreatic cancer triples if a person's mother, father, sister, or brother had the disease. Also, a family history of colon or ovarian cancer increases the risk of pancreatic cancer.
Chronic pancreatitis - Chronic pancreatitis is a painful condition of the pancreas. Some evidence suggests that chronic pancreatitis may increase the risk of pancreatic cancer.
Other studies suggest that exposure to certain chemicals in the workplace or a diet high in fat may increase the chance of getting pancreatic cancer.
Most people with known risk factors do not get pancreatic cancer. On the other hand, many who do get the disease have none of these factors. People who think they may be at risk for pancreatic cancer should discuss this concern with their caregiver. They may suggest ways to reduce the risk and can plan a sensible schedule for checkups.
Symptoms
Pancreatic cancer is sometimes called a "silent disease" because early pancreatic cancer often does not cause symptoms.
But, as the cancer grows, symptoms may include:

Weakness
Abdominal pain
Diarrhea
Depression
Loss of appetite
Indigestion
Pain in the upper abdomen or upper back
Nausea and vomiting
Jaundice
Back pain
Yellow skin and eyes, and dark urine from jaundice
Weight loss
Fatigue
Clay-colored stools
Thrombophlebitis or unexplained blood clots
These symptoms are not sure signs of pancreatic cancer. Other problems can also cause these symptoms. Anyone with these symptoms should see a doctor so that the problems may be treated as early as possible.
Diagnosis
If a patient has symptoms that suggest pancreatic cancer, the doctor asks about the patient's medical history. The doctor may perform a number of procedures, including one or more of the following:
Physical exam - Your skin and eyes will be examined for signs of jaundice. Then the abdomen is checked for changes in the area near the pancreas, liver, and gallbladder. It is also checked for ascites, an abnormal buildup of fluid in the abdomen.
Lab tests - The caregiver may take blood, urine, and stool samples to check for bilirubin and other substances. Bilirubin is a substance that passes from the liver to the gallbladder to the intestine. If the common bile duct is blocked by a tumor, the bilirubin cannot pass through normally. Blockage may cause the level of bilirubin in the blood, stool, or urine to become very high. High bilirubin levels can result from cancer or from non-cancerous conditions.
CT scan (Computed tomography) - An x-ray machine linked to a computer takes a series of detailed pictures. The x-ray machine is shaped like a donut with a large hole. The patient lies on a bed that passes through the hole. As the bed moves slowly through the hole, the machine takes many x-rays. The computer puts the x-rays together to create pictures of the pancreas and other organs and blood vessels in the abdomen.
Ultrasonography - The ultrasound device uses sound waves that cannot be heard by humans. The sound waves produce a pattern of echoes as they bounce off internal organs. The echoes create a picture of the pancreas and other organs inside the abdomen. The echoes from tumors are different from echoes made by healthy tissues. The ultrasound procedure may use an external or internal device, or both types:
Transabdominal ultrasound: To make images of the pancreas, the doctor places the ultrasound device on the abdomen and slowly moves it around.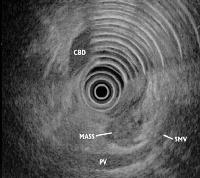
EUS (Endoscopic ultrasound): The caregiver passes a thin, lighted tube (endoscope) through the patient's mouth and stomach, down into the first part of the small intestine. At the tip of the endoscope is an ultrasound device. The caregiver slowly withdraws the endoscope from the intestine toward the stomach to make images of the pancreas and surrounding organs and tissues.
ERCP (endoscopic retrograde cholangiopancreatography) - The caregiver passes an endoscope through the patient's mouth and stomach, down into the first part of the small intestine. The doctor slips a smaller tube (catheter) through the endoscope into the bile ducts and pancreatic ducts. After injecting dye through the catheter into the ducts, the doctor takes x-ray pictures. The x-rays can show whether the ducts are narrowed or blocked by a tumor or other condition.
PTC (percutaneous transhepatic cholangiography) - A dye is injected through a thin needle inserted through the skin into the liver. Unless there is a blockage, the dye should move freely through the bile ducts. The dye makes the bile ducts show up on x-ray pictures. From the pictures, the doctor can tell whether there is a blockage from a tumor or other condition.
Biopsy - In some cases, tissue may be removed. A pathologist (doctor specialized in looking at tissue samples) then uses a microscope to look for cancer cells in the tissue. This may be done in several ways. One way is by inserting a needle into the pancreas to remove cells. This is called fine-needle aspiration. The caregiver uses x-ray or ultrasound to guide the needle. Sometimes a sample of tissue is obtained during EUS or ERCP (as described above). Another way is to open the abdomen during an operation.
Staging
When pancreatic cancer is diagnosed, the doctor needs to know the stage, or extent, of the disease to plan the best treatment. Staging is a careful attempt to find out the size of the tumor in the pancreas, whether the cancer has spread, and if so, to what parts of the body.
The doctor may determine the stage of pancreatic cancer at the time of diagnosis, or the patient may need to have more tests. Such tests may include blood tests, a CT scan, ultrasonography, laparoscopy, or angiography. The test results will determine which treatment is best.
Treatment
Many people with pancreatic cancer want to take an active part in making decisions about their medical care. They want to learn all they can about their disease and their treatment choices. However, the shock and stress that people may feel after a diagnosis of cancer can make it hard for them to think of everything they want to ask the doctor. Often it helps to make a list of questions before an appointment. To help remember what the caregiver says, patients may take notes or ask whether they may use a tape recorder. Some patients also want to have a family member or friend with them when they talk to the doctor to take part in the discussion, to take notes, or just to listen.
Cancer of the pancreas is very hard to control with current treatments. For that reason, many doctors encourage patients with this disease to consider taking part in a clinical trial. Clinical trials are an important option for people with all stages of pancreatic cancer.
At this time, pancreatic cancer can be cured only when it is found at an early stage, before it has spread. However, other treatments may be able to control the disease and help patients live longer and feel better. When a cure or control of the disease is not possible, some patients and their doctors choose palliative therapy. Palliative therapy aims to improve quality of life by controlling pain and other problems caused by this disease, but does not cure the disease.
The doctor may refer patients to an oncologist, a doctor who specializes in treating cancer, or patients may ask for a referral. Specialists who treat pancreatic cancer include surgeons, medical oncologists, and radiation oncologists. Treatment generally begins within a few weeks after the diagnosis. There will be time for patients to talk with the caregiver about treatment choices, get a second opinion, and learn more about the disease.
Methods of Treatment
People with pancreatic cancer may have several treatment options. Depending on the type and stage, pancreatic cancer may be treated with surgery, radiation therapy, or chemotherapy. Some patients have a combination of therapies.
Surgery may be used alone or in combination with radiation therapy and chemotherapy. At the time of diagnosis, only about 20% of pancreatic tumors can be removed by surgery. The standard procedure is called a pancreaticoduodenectomy (Whipple procedure). This surgery for pancreatic cancer should be done at centers that perform the procedure frequently. The surgeon may remove all or part of the pancreas. The extent of surgery depends on the location and size of the tumor, the stage of the disease, and the patient's general health. Brief descriptions of procedures are as follows:
Whipple procedure: If the tumor is in the head (the widest part) of the pancreas, the surgeon removes the head of the pancreas and part of the small intestine, bile duct, and stomach. The surgeon may also remove other nearby tissues.
Distal pancreatectomy: The surgeon removes the body and tail of the pancreas if the tumor is in either of these parts. The surgeon also removes the spleen.
Total pancreatectomy: The surgeon removes the entire pancreas, part of the small intestine, a portion of the stomach, the common bile duct, the gallbladder, the spleen, and nearby lymph nodes.
Sometimes the cancer cannot be completely removed. But if the tumor is blocking the common bile duct or duodenum, the surgeon can create a bypass by placing a biliary stent (similar to stents placed in the arteries of the heart to relieve blockages) during ERCP. In this procedure your caregiver uses an endoscope to place a stent in the blocked area. A stent is a tiny plastic or metal mesh tube that helps keep the duct or duodenum open.
After surgery, some patients are fed liquids intravenously (by IV) and through feeding tubes placed into the abdomen. Patients slowly return to eating solid foods by mouth. A few weeks after surgery, the feeding tubes are removed.
These are some questions a person may want to ask the caregiver before having surgery:
What kind of operation will I have?
How will I feel after the operation?
How will you treat my pain?
What other treatment will I need?
How long will I be in the hospital?
Will I need a feeding tube after surgery? Will I need a special diet?
What are the long-term effects?
When can I get back to my normal activities?
How often will I need checkups?
When the tumor is confined to the pancreas but cannot be removed, a combination of radiation therapy and chemotherapy may be recommended. When the tumor has spread (metastasized) to other organs such as the liver, chemotherapy alone is usually used.
Radiation therapy (also called radiotherapy) uses high-energy rays to kill cancer cells. A large machine directs radiation at the abdomen. Radiation therapy may be given alone, or with surgery, chemotherapy, or both.
Radiation therapy is local therapy. It affects cancer cells only in the treated area. For radiation therapy, patients go to the hospital or clinic, often 5 days a week for several weeks.
Doctors may use radiation to destroy cancer cells that remain in the area after surgery. They also use radiation to relieve pain and other problems caused by the cancer.
These are some questions a person may want to ask the caregiver before having radiation therapy:
Why do I need this treatment?
When will the treatments begin? When will they end?
How will I feel during therapy? Are there side effects?
What can I do to take care of myself during therapy? Are there certain foods that I should eat or avoid?
How will we know if the radiation is working?
Will I be able to continue my normal activities during treatment?
Chemotherapy is the use of drugs to kill cancer cells. Caregivers also give chemotherapy to help reduce pain and other problems caused by pancreatic cancer. It may be given alone, with radiation, or with surgery and radiation.
Chemotherapy is systemic therapy. The caregiver usually gives the drugs by injection. Once in the bloodstream, the drugs travel throughout the body.
Usually chemotherapy is an outpatient treatment given at the hospital, clinic, doctor's office, or home. However, depending on which drugs are given and the patient's general health, the patient may need to stay in the hospital.
Patients may want to ask these questions about chemotherapy:
Why do I need this treatment?
What will it do?
What drugs will I be taking? How will they be given? Will I need to stay in the hospital?
Will the treatment cause side effects? What can I do about them?
How long will I be on this treatment?
Side effects of treatment
Because cancer treatment may damage healthy cells and tissues, unwanted side effects are common. These side effects depend on many factors, including the type and extent of the treatment. Side effects may not be the same for each person, and they may even change from one treatment session to the next. The health care team will explain possible side effects and how they will help the patient manage them.
Surgery
Surgery for pancreatic cancer is a major operation. Patients need to stay in the hospital for several days afterward. Patients may feel weak or tired. Most need to rest at home for about a month. The length of time it takes to regain strength varies.
The side effects of surgery depend on the extent of the operation, the person's general health, and other factors.
Most patients have pain for the first few days after surgery. Pain can be controlled with medicine, and patients should discuss pain relief with the doctor or nurse.
Removal of part or all of the pancreas may make it hard for a patient to digest foods. The health care team can suggest a diet plan and medicines to help relieve diarrhea, pain, cramping, or feelings of fullness. During the recovery from surgery, the doctor will carefully monitor the patient's diet and weight. At first, a patient may have only liquids and may receive extra nourishment intravenously or by feeding tube into the intestine. Solid foods are added to the diet gradually.
Patients may not have enough pancreatic enzymes or hormones after surgery. Those who do not have enough insulin may develop diabetes. The caregiver can give the patient insulin, other hormones, and enzymes.
Radiation Therapy
Radiation therapy may cause patients to become very tired as treatment continues. Resting is important, but caregivers usually advise patients to try to stay as active as they can.
When patients receive radiation therapy, the skin in the treated area may sometimes become red, dry, and tender.
Radiation therapy to the abdomen may cause nausea (feeling sick to your stomach), vomiting, diarrhea, or other problems with digestion. The health care team can offer medicine or suggest diet changes to control these problems.
For most patients, the side effects of radiation therapy go away when treatment is over.
Chemotherapy
The side effects of chemotherapy depend mainly on the drugs and the doses the patient receives as well as how the drugs are given. In addition, as with other types of treatment, side effects vary from patient to patient.
Systemic chemotherapy affects rapidly dividing cells throughout the body, including blood cells. Blood cells fight infection, help the blood to clot, and carry oxygen to all parts of the body. When anticancer drugs damage healthy blood cells, patients are more likely to get infections, may bruise or bleed easily, and may have less energy.
Cells in hair roots and cells that line the digestive tract also divide rapidly. As a result, patients may lose their hair and may have other side effects such as poor appetite, nausea and vomiting, diarrhea, or mouth sores.
Usually, these side effects go away gradually during the recovery periods between treatments or after treatment is over. The health care team can suggest ways to relieve side effects.
Prognosis
When pancreatic cancer can be surgically removed, cure may be expected. However, cure rates may be less than 50%. Chemotherapy and radiation are often given after surgery to attempt to increase the cure rate. For pancreatic cancer that cannot be removed completely with surgery, or cancer that has spread beyond the pancreas, cure is not currently possible. Always remember that statistics are numbers and chances, and that each case is individual.
Complications
Pancreatic cancer may result in weight loss, blood clots, liver dysfunction, infections, pain, and depression. Symptoms such as pain can usually be controlled with aggressive pain management.
Prevention
If you smoke, stop smoking. Eat a diet high in fruits, vegetables, and whole grains, and exercise regularly.