Gallbladder polyps

What are Gallbladder polyps?
Lesions that project from the gallbladder wall into the gallbladder interior are called gallbladder polyps (GPs). In the majority of patients, diagnosis is an incidental finding of a routine abdominal ultrasound or following cholecystectomy for gallstones or biliary colic. Even though most of the gallbladder polyps are benign in nature, malignant polyps are present in some cases, and early detection and appropriate early measure is important for curative treatment and long-term survival. The primary goal in the management of gallbladder polyps is to prevent the development of gallbladder carcinoma.
Gallbladder polyps are classified as benign or malignant. Benign GPs are subdivided into: pseudotumors (cholesterol polyps, inflammatory polyps; cholesterolosis and hyperplasia), epithelial tumors (adenomas) and mesenchymatous tumors (fibroma,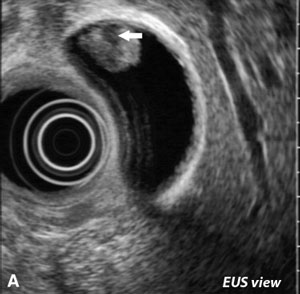 lipoma, and hemangioma). Malignant GPs are gallbladder carcinomas.
lipoma, and hemangioma). Malignant GPs are gallbladder carcinomas.
The poor prognosis of gallbladder carcinoma patients means it is important to differentiate between benign polyps and malignant or premalignant polyps.
Cholesterol polyps
Recent studies have shown that the majority of gallbladder polyps are benign, and 60–90% of them are cholesterol polyps. Cholesterol polyps are generally less than 10 mm. often multiple cholesterol polyps are present
Inflammatory polyps
Inflammatory polyps are uncommon. They account for about 10% of gallbladder polyps and result from granulation and fibrous tissue secondary to chronic inflammation. They are typically less than 10 mm in size and are not neoplastic.
Gallbladder adenomas
Although adenomas are benign polyps, they can exhibit premalignant behavior. These lesions are habitually pedunculated single lesions and may be associated with gallstones or chronic cholecystitis. They range in size from 5 to 20 mm and are generally solitary. Gallbladder adenomas are rare, but well-documented benign epithelial tumors.
Adenomyomatosis
Adenomyomatosis, a noninflammatory gallbladder alteration, occurs in middle age patients, and the incidence increases with age. Originally depicted as a benign finding, it is currently identified as a precancerous lesion.
Symptomatology
The presenting symptoms of polypoid lesions of the gallbladder are nonspecific and vague, and in many cases asymptomatic. For such reason, polypoid lesions of the gallbladder are often detected incidentally. However, there are some patients with gallbladder polyps which may suffer nausea, vomiting, and occasional pain in the right hypochondrium.
Polyps are sometimes identified on transabdominal ultrasounds done for right upper quadrant pain. In the absence of other findings, the gallbladder polyp may be considered a source of biliary colic. If any symptoms are caused, most commonly right upper quadrant pain, nausea, dyspepsia, and jaundice are seen.
Symptoms may be associated with pseudo-polyps such as a cholesterol polyp, inflammatory or hyperplastic polyp, which include indigestion, right upper quadrant pain, and discomfort, cholecystitis or gallbladder stone. Metabolic syndrome has a close relationship with the development of cholesterol polyps.
Incidence of gallbladder polyps
The prevalence of gallbladder polyps was reported as 4.3–6.9%. Polypoid gallbladder lesions include a variety of pathologic types. Although there are some differences according to reports, the prevalence of polypoid lesions of the gallbladder are reported in 2–12% of cholecystectomy specimens. The sex ratio and age at the time of diagnosis of gallbladder polyps was 1.15 to 1 (male to female)
Proposed patient risk factors for malignant gallbladder polyps include age greater than 60, presence of gallstones, and primary sclerosing cholangitis. Polyp risk characteristics include a size greater than 6 mm, solitary, and sessile.
Relation between gallbladder stones and gallbladder polyps
Some patients who are confirmed to have polypoid lesions of the gallbladder through cholecystectomy are associated with gallstone. Symptomatic cases tended to increase with the increase in polyp size.
Imaging of gallbladder polyps
Ultrasonography
Abdominal ultrasound is looked upon as the best available exam for diagnosing gallbladder polyps, not only because of its accessibility and low cost, but also because of its good sensitivity and specificity. The polyps can be located, counted, and measured with ultrasound, and the three layers of the gallbladder wall and any abnormalities can be viewed. The polyps appear as fixed, hyperechoic material protruding in to the lumen of the gallbladder. Generally, polyps in the gallbladder are demonstrable on US, only when they are over 5 mm in diameter. Sonographic differentiation between benign and malignant polyps (and calculous disease) relies greatly on the size of a single nonmobile lesion within the gall bladder. A gallstone impacted within the gallbladder wall may be easily mistaken for a polyp on ultrasound scanning.
Three-dimensional ultrasonography
Three-dimensional ultrasound (3DUS) diagnosis correlates well with two-dimensional ultrasound (2DUS) with regard to most gallbladder problems and could be sufficient as a stand-alone technique.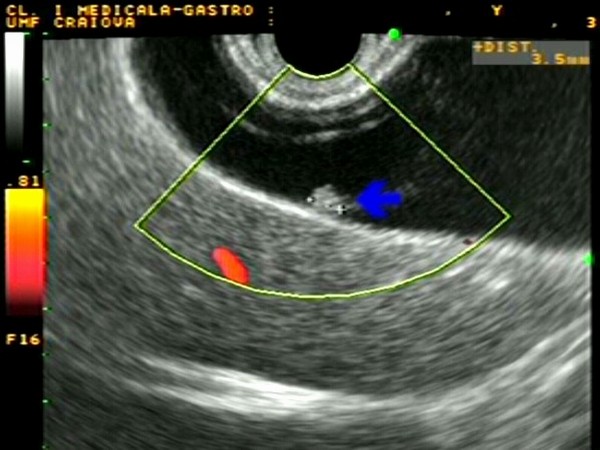 (EUS) Endoscopic ultrasonography
(EUS) Endoscopic ultrasonography
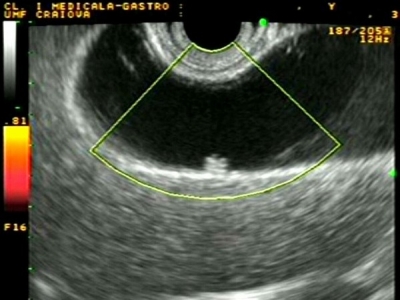
Endoscopic ultrasonography (EUS) was considered the most sensitive diagnostic modality for gallbladder polypoid lesions. However, the diagnostic accuracies of high-resolution ultrasound EUS for the differential diagnosis of gallbladder polypoid lesions are very high. In view of patient comfort is considered that Endoscopic ultrasonography EUS is likely to become an important diagnostic modality for the differential diagnosis and staging of gallbladder polypoid lesions and early gallbladder cancer.
Clinical series, indications for surgery, and recommended follow-up.
Any gallbladder polyp that is felt to be symptomatic should be removed. In patients at risk for malignancy, a polyp of 6 mm or greater should likely be resected. Patients without risk factors are good candidates for EUS for further evaluation. Those polyps that are considered high risk by EUS criteria should be considered for resection.
 The cholecystectomy should only be undertaken in cases where there are clinical signs of gallbladder polyps, polyps with diameters greater than 10 mm, fast-growing polyps, sessile polyps or wide-based polyps, polyps with long pedicles, patient aged over 50, concurrent gallstones, polyps of the gallbladder in fundibulum or abnormal gallbladder wall ultrasound.
The cholecystectomy should only be undertaken in cases where there are clinical signs of gallbladder polyps, polyps with diameters greater than 10 mm, fast-growing polyps, sessile polyps or wide-based polyps, polyps with long pedicles, patient aged over 50, concurrent gallstones, polyps of the gallbladder in fundibulum or abnormal gallbladder wall ultrasound.
The surgery of choice is laparoscopic cholecystectomy. A gallbladder polyp greater than 18 mm in size has a high likelihood of being an advanced cancer; it should be removed with open cholecystectomy, partial liver resection, and possible lymph node dissection.[8]
Gallbladder polyps that are not resected should be followed-up with serial ultrasound examinations. Clear guidelines on a screening interval are so far not available, even though a screening interval of every 6–12 months has been documented.
Clinical recommendations
In patients with age ≥60 years, sessile polyp morphology, and polyp size ≥10 mm, a generous approach to EUS for closer characterization should be the normal. In all cases where there are indications of malignancy, a cholecystectomy should be recommended.
If there are no signs of malignancy, a follow-up with the same modality is done after 6 months. If by 6 months there is no changes in size, contour, or vascualrity, the follow-up should be individualized – most often a follow-up after another 12 months could be recommended.
For polyps 6–9 mm in diameter without signs of malignancy, a new US is recommended after 6 months. If the does not show any significant changes a new US is recommended after another 12 months and if no changes is found than no further imaging studies are made. Gallbladder polyps smaller than 6 mm are not followed up, if there are no indications of malignancy.